Two readers recently asked about Total Knee Arthroplasty/Replacements and how you would go about treating them without causing pain.
Let's review a great blog post by my colleague Dr. Joe Brence, regarding the best predictor of success in a long term follow up for TKA. In case you did not click the link, it's fear avoidance, not strength, ROM, prior function, etc.
An example I use in many of my courses is the one that most of us have gone through on Acute Care internships. My first affiliation was in an Acute Care setting and one of my first patients was a sweet little old lady who just had a TKA. I was lightly stretching her and she told me how much it hurt. My CI simply stated, "Sorry Mrs. X, we have to get you to 90!" She then pulled me aside and told me how hard Mrs. X's recovery and quality of life would be if we did not get her to 90 pain or no, WHATEVER THE COST!" Ok, well she didn't really say that last part, but I think early on in our pre-careers we learn that it's ok and even necessary to cause pain as a means to an end.
One on of my last internships, I had the opportunity to watch 2 TKAs, I remember the surgeon, upon finding out I was a PT student ask me, "Look, after I'm done, they have full ROM." Then he ranged the knee easily and fully into extension and flexion. He then asked, "How come after I send them to you guys, they have such limited range?"
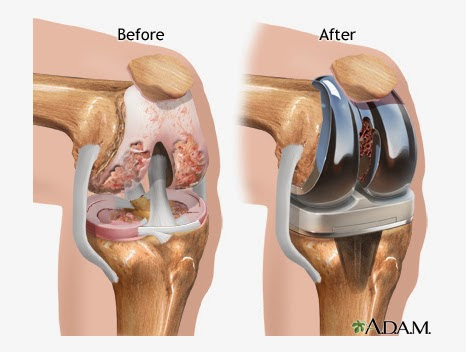
I really wanted to say, "How would you feel if someone just sawed off the ends of your femur and tibia, then used a big mallet to pound in the new prostheses, then sewed you back up?" Seriously, it was quite obvious to me back then. However, the take home for us all is that when unconscious, there is FULL ROM. It is only upon waking when both the chemical inflammatory mediators combined with the threat perception from the CNS take over.
This is why CPM does not work, it probably hurts like heck and does nothing to alleviate anxiety. Knowing that a majority of your patients actually have the requisite ROM needed for function, there is really no point on cranking on them "to prevent scar tissue" or "break up scar tissue." This is what I do for these cases, that normally results in most of their range, strength, and function restored (even on B TKAs) in around 12 visits on average.
- very light IASTM to the anterior thigh, posterior thigh, anterior and posterior lower legs, but staying clear of the incision
- light EDGE Mobility Band wrapping to help decrease threat during movement
- very light passive ranging and encouraging active assistance
- HEP is mini lunges, mini squats, step ups and downs and frequent movement in the pain free range
- that pain free range is very important, you want to reduce threat, not increase with painful passive stretching
- encourange them tell the patient their brain is doing a good job protecting the new joint, and pain/discomfort is normal
- the range and function will come with some frequent movement, and gradual exposure to WB
- regression to NWB exercises only if the patient is in so much pain they cannot perform WB (unlikely unless they come directly to your clinic and skip sub-acute)
It really sounds like I reiterate the same point every week, but it cannot be overstated. You do not have to cause pain (or increase existing pain) on ANY patient to get results. Of course a TKA procedure is going to cause pain. That is a given. There are of course hardy patients who can take a beating, but you cannot "force" increased range until the nervous system is ready for it.
Keeping it Eclectic..











Post a Comment
Post a Comment